What makes resting heart rate decrease?
Does it come from inside or outside the heart?
By far the easiest exercise adaptation to measure is your resting heart rate (RHR). It doesn’t even require any technology, but we do have great devices now to measure it and you’re probably wearing one right now. An untrained person will have a RHR of about 70 beats per minute (bpm). If you’re pretty trained, that can decrease by 30-40 beats, without even being an elite athlete. When I’m sleeping my RHR is regularly 31-34 bpm.
But how does it actually decrease in a physiological sense? What’s going on under the hood?
The Heart’s Nervous System
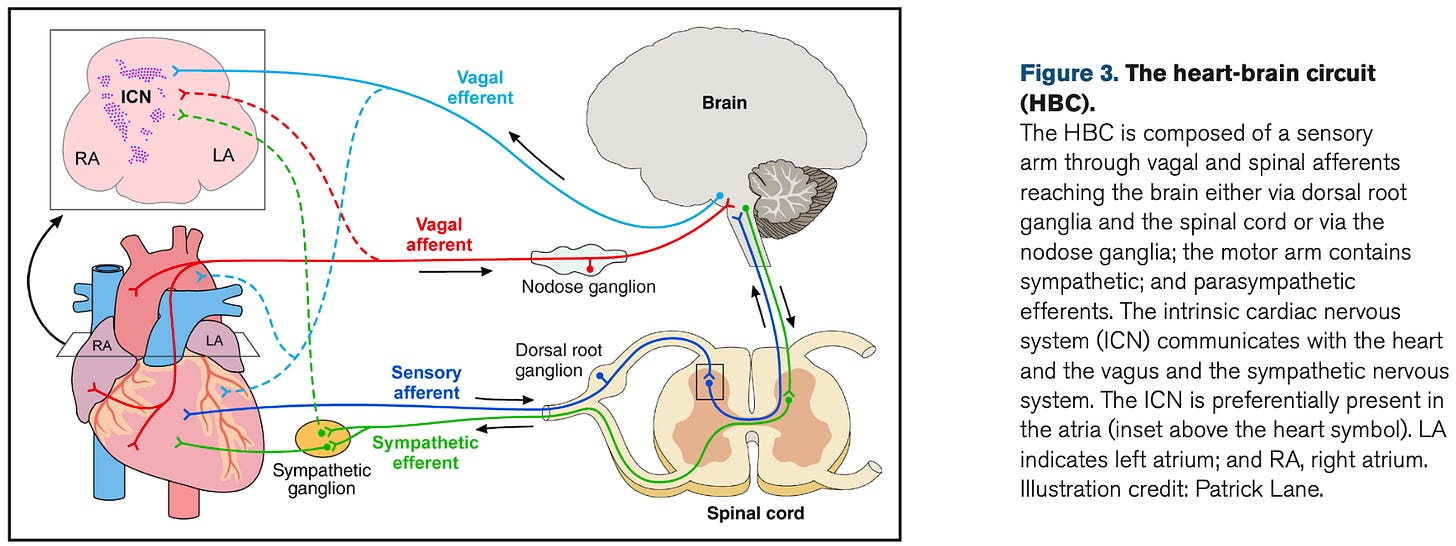
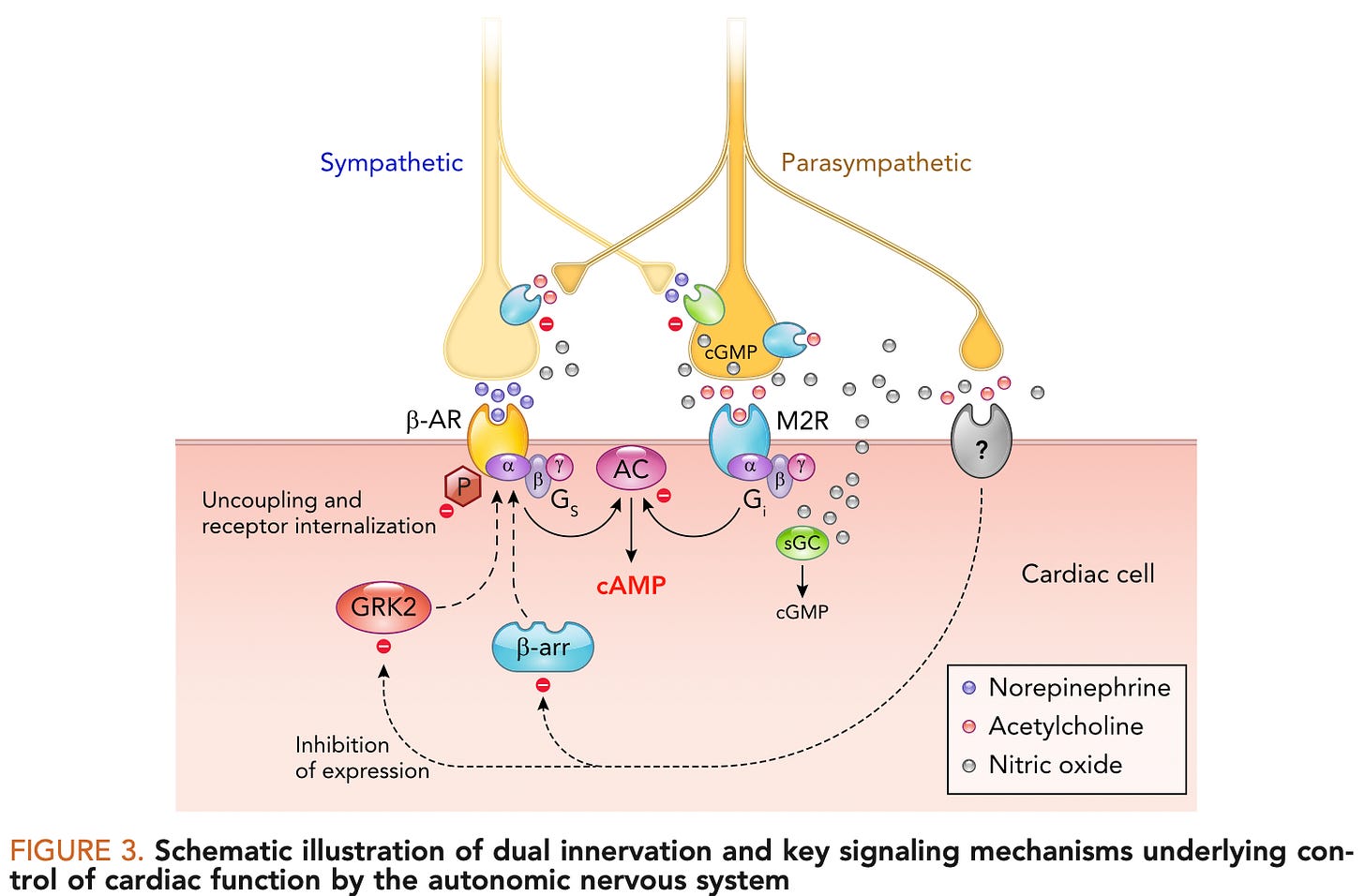
Two types of nerves innervate the heart, sympathetic (the gas pedal; increases heart rate) and parasympathetic (the brakes, decreases heart rate, also known as vagal nerves). These nerves are like two dimmer switches controlling the same light and we are constantly toggling between sympathetic or parasympathetic predominance.
When we exercise or are stressed (physically, emotionally, mentally), the sympathetic switch ramps up and the parasympathetic switch turns down. Actually, when we first start running the parasympathetic switch turns down before the sympathetic one turns up, referred to as parasympathetic withdrawal.
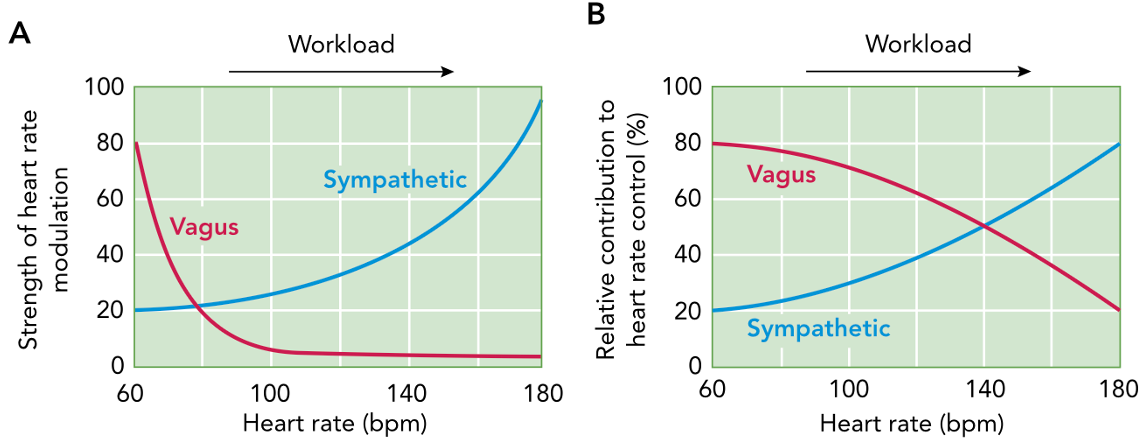
But what is controlling the switches?
Our brain does its fair share. Some of these nerves have a direct path from the brain to the heart. Just thinking about exercise will increase heart rate (pre-race jitters). This is also why mental or emotional stress alter heart rate (up or down), and can cause fainting which is often due to the so-called vaso-vagal response (vaso = dilate blood vessels, vagal = decreased heart rate).
The nerves can also go in the reverse direction, from the heart to the brain. The heart can sense low oxygen or increased pressure, for example, relays that information upstairs, then the brain sends signals back that increase or decrease heart rate.
But what are the signals?!
They’re basically electrical currents that zoom down the nerves at incredible speeds, as quick as 11.5 meters per second (26 mph) in one study and 16.4 meters per second in another. When you consider how close your heart is to your brain, it’s easy to see realize how quick these effects can happen (milliseconds).
When these currents reach their destination (the heart, and others), they release chemicals. The parasympathetic nerves release acetylcholine which slows heart rate. Drugs like atropine block acetylcholine and increase heart rate. Sympathetic nerves release norepinephrine (also known as noradrenaline) which increases heart rate. Beta-blocker drugs block norepinephrine and decrease heart rate.
Sympathetic nerve activity is important to ramp ourselves up during exercise, but other than that we want more input from the parasympathetic side. Excess sympathetic activity is notable in many disease states.
The Effect of Training
A lower RHR as we get more fit can be explained by 2-3 things.
Higher stroke volume
Increased parasympathetic activity (also known as vagal tone)
Decreased intrinsic heart rate
Number 1 is pretty easy. If a heart pumps more blood per heart beat you simply don’t need as many beats. But that’s not necessarily why it decreases.
Number 2 is probably the most accepted mechanism. Those nerves in the brain sending signals to the heart are literally more active (more electricity). Most people measure this with the [imperfect] heart rate variability measure. Higher HRV usually means higher parasympathetic activity. In my opinion, resting HR is mostly just as useful as resting HRV, but nonetheless it is a decent marker.
A good way to illustrate this is a study in dogs, who are often used in invasive cardiovascular research because of a better relationship to humans than mice/rats. After 3 months of training, resting and exercising heart rate decreased substantially as expected, compared to non-exercisers. They repeated the same heart rate tests but administered drugs to block both types of nerves in the heart, and this time there was no difference between groups, meaning that the reductions in heart rate were solely due to enhanced parasympathetic nerve activity. Studies in humans after 8 months of training, and comparing athletes to non-athletes, find similar results.
Number 3 is a bit contentious. We have an intrinsic heart rate set by the sinoatrial (SA) node. Everyone’s heart has one and this sets our heart rate at 100 beats per minute. It’s our built in pacemaker. If I took your heart out of your chest it would still beat 100 times per minute.
You might then wonder why you’re resting heart rate isn’t simply 100 bpm. Weird.
It’s because the parasympathetic nerve activity and acetylcholine overrides the pacemaker. Fortunately we don’t have to take your heart out of your chest to test your intrinsic heart rate. That’s why the study I mentioned above used drugs to block the heart’s nervous system. When you remove that input, the heart rate you get is presumably due to the pacemaker, and it’s pretty much exactly 100 bpm.
Some scientists think getting more fit decreases the intrinsic heart rate below 100, and they have data to back it up. Runners, rowers, and cyclists all seem to have a slower pacemaker. These were not training studies though where they measured them before and after they “became athletes”. They were snapshots in time of highly fit athletes and regular people of a similar age.
This is an important point because it means you can’t rule out a potential genetic component. It could also mean that training might cause your pacemaker to slow, but only after years of high volume, high intensity training that athlete’s do and wouldn’t be captured in an exercise study of only a few weeks/months. How the pacemaker actually slows down is a whole other topic. It might involve metabolic changes in ion channels within the heart, which is hard to directly measure in humans and a bit complex.
Physiology is Rarely Binary
You can read about the debate between the two mechanisms here. Parasympathetic activity without a doubt increases with exercise training and contributes to a lower RHR. But, years of hard training may also eventually slow your built-in pacemaker. There seems to be a genetic influence on RHR as well which is linked to atrial fibrillation (lower RHR, higher a-fib risk). Lifelong endurance athletes are known to be at risk for a-fib. There’s no data yet to suggest their low RHR is a reason for why they get a-fib, but understanding the mechanisms of decreased heart rate might be helpful for developing prevention strategies or treatments.
Some References
Immediate and sustained increases in the activity of vagal preganglionic neurons during exercise and after exercise training. Cardiovascular Research, 2023.
Exercise training-induced bradycardia: evidence for enhanced parasympathetic regulation without changes in intrinsic sinoatrial node function. Journal of Applied Physiology, 2015.
Exercise training reduces resting heart rate via downregulation of the funny channel HCN4. Nature communications, 2014.
Sean Langan has his PhD in exercise physiology. He is interested in how exercise training rewires our biology and harnessing the intersection of human physiology, technology, research, and coaching to improve human performance.