An Overview of Histamine
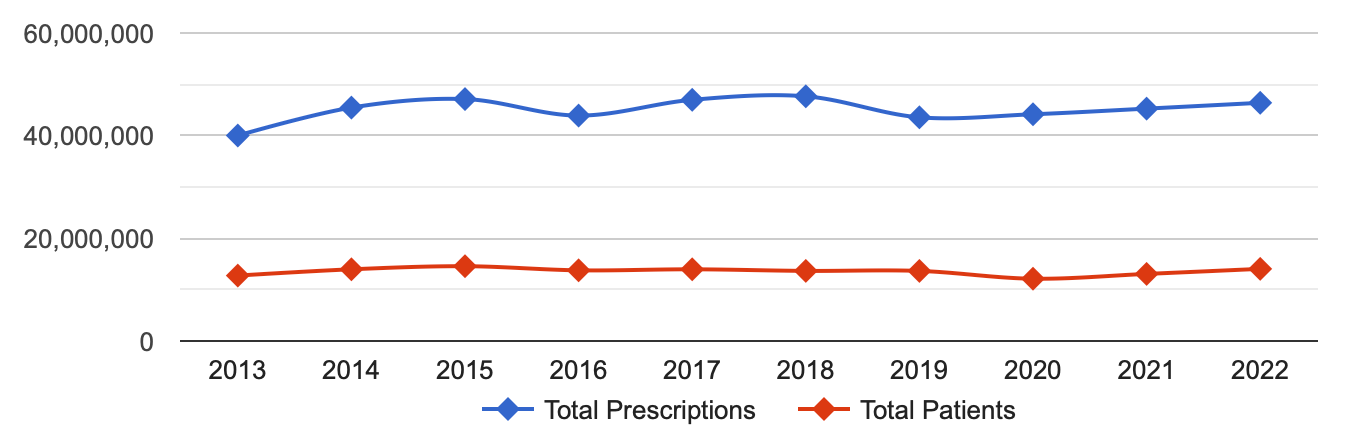
Histamine is most famous as a chemical responsible for allergic reactions, like sneezing. It’s a healthy part of our immune response, but sometimes those symptoms can get unbearable and we want to tone them down. Enter anti-histamines. In the US we take quite a bit of them, about 40-50 million prescriptions per year.
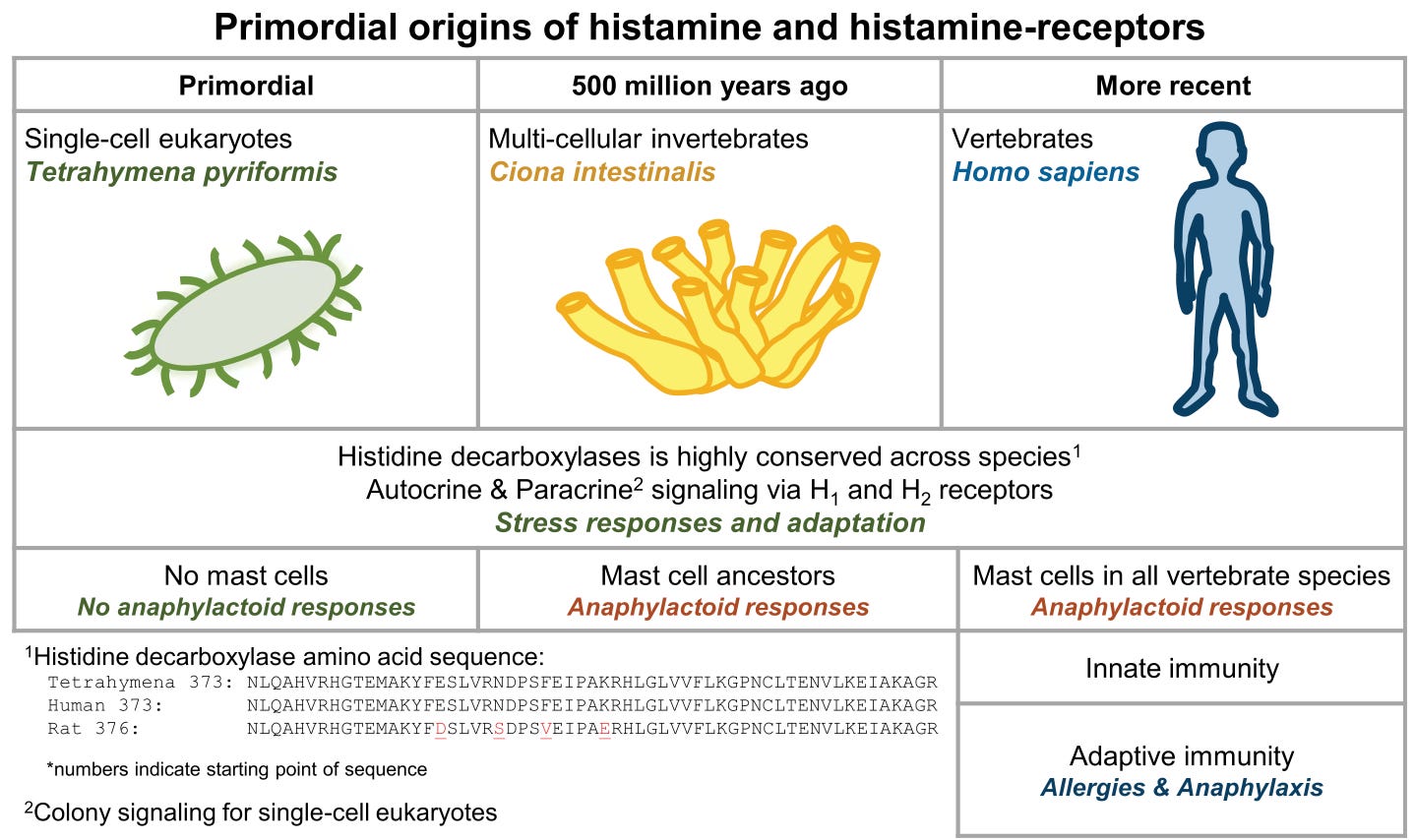
Interestingly, histamine does more than just our immune response. You can find the gene for histidine decarboxylase (which produces histamine) in single-celled organisms that were around long before an immune system as we know it existed.
That histamine-producing enzyme, histidine decarboxylase exists in several cell types, most notably mast cells. When activated and histamine production ramps up, it binds to histamine receptors (H1, H2, H3, H4) which are located throughout the body to exert its physiological effects. Anti-histamine drugs work by blocking histamine from interacting with those receptors.
The Give and Take of Physiology
The thing about human physiology is that nothing is free. Take mouthwash as an example. As far as I’m concerned, it’s pretty good for your mouth health, but it does kill beneficial oral bacteria, some of which help produce nitric oxide. Studies even find mouthwash use is linked to high blood pressure, and if you're taking beet root juice I would stay away from the mouthwash.
Is the same true for anti-histamines? Benadryl can make us drowsy, but might there be other side effects?
Beyond Allergies
Histamine and Blood Vessels
As I was working on my dissertation focused on how our vascular system adapts to exercising in the heat, I had to read up on the biochemical signals responsible for vasodilation of blood vessels. You know, like nitric oxide (of beet root juice fame). Histamine also makes the list as vasodilation is part of the immune response, and people with severe allergic reactions can develop dangerously low blood pressure.
How is that? H1 and H2 receptors exist in vascular cells within skeletal muscles. In the early 80’s, a petri-dish study as I like to call it, found that adding histamine to human vascular cells performs a hockey assist and increases production of a potent vasodilator, ultimately resulting in relaxation of blood vessels.
In intact humans, people noticed histamine went up in the blood after exercise and you might be able to block the increase in blood flow with anti-histamines (H1/H2 receptor antagonists). This was interesting because it suggests histamine may be controlling blood flow in conditions beyond just allergic reactions.
In the last 10 years or so, careful studies have found that histamine plays a big role in the “aftereffects” of exercise. When we finish exercising our heart stops pumping blood at a high rate (and pressure) pretty quickly, but blood flow in those active leg muscles stays elevated for several hours (post-exercise vasodilation). This mismatch between the heart and blood vessels can produce hypotension and potentially that wobbly, lightheaded feeling leading to a collapse because those dilated leg blood vessels don’t get enough blood back up to the heart quick enough.
Histamine controls a large portion of this elevated blood flow. When you block both H1 and H2 histamine receptors, you can nearly get rid of all the post-exercise vasodilation, and the enzyme responsible for histamine release from mast cells is elevated in marathoners who collapsed versus those who didn’t.
Effects on Metabolism and Gene Expression
In 2016 a group of scientists wanted to see if these vascular changes from blocking histamine are reflected in changes in how genes are expressed in our muscle. Exercise tells genes to do more or less of its intended job. For example, a gene responsible for muscle growth will be turned up (increased gene expression) with strength training.
They were mainly concerned with vascular-related genes and found that normal exercise (one session) changed the expression of ~3,000 genes (either up or down). That in of itself is nothing new.
Taking an anti-histamine before exercise resulted in only ~1,000 genes changing. It was a pretty big clue that histamine was important in controlling cellular responses to exercise and blocking it took away some of the benefits.
In the authors words, histamine left a broad “footprint” on exercising muscle.
Relevance?
At this point, I thought this stuff was interesting science, but that’s about it. Although I hardly ever take allergy medication, it wasn’t because I thought it would interfere with my exercise. It’s usually just never bad enough to warrant a trip to the pharmacy.
Muscle Glycogen Replenishment
In April, a new study piqued my interest some more, showing an extensive cellular communication network involving histamine during and after exercise. The important differentiator from allergies is that histamine goes up in the muscle’s interstitial fluid (fluid between cells) but not systemically in the blood, confining its effects locally.
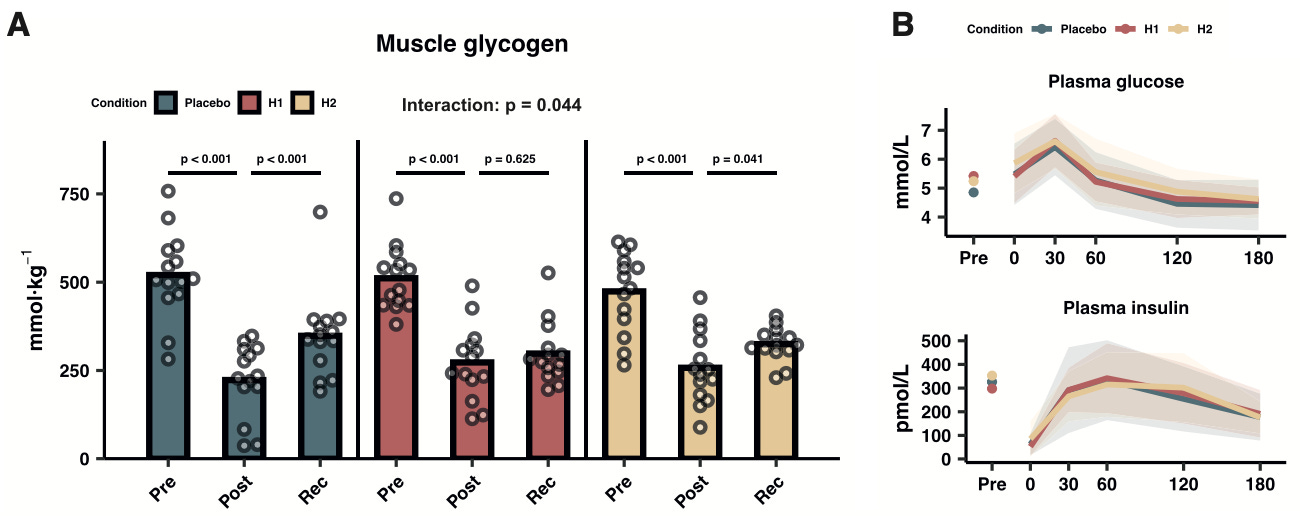
The part I want to harp on is regarding muscle glycogen. They had people do a ~1 hour interval training session (7 x 3min on / 3min off with warm up and cool down) and took muscle biopsies before, immediately after, then 3 hours later, to see how much glycogen they used during exercise and were able to replenish afterwards. They either got placebo, or an anti-histamine blocking the H1 or H2 receptor (see picture).
Everyone used up about half of their muscle glycogen from the exercise. Three hours later, the control and H2-antihistamine (famotidine) group increased muscle glycogen by about 25-30%, but the group with the H1-antihistamine (fexofenadine) had no change despite eating the same amount. They all might have been back to normal the following morning (we don’t know), but if you’re training multiple times a day, that short-term replenishment is important and could be a reason to avoid anti-histamines surrounding exercise sessions.
Chronic Exercise Training
Two separate 6-week studies from 2021 and 2025 (April) have looked at whether anti-histamines interfere with exercise adaptations. VO2max didn’t change but there was a slight benefit for the placebo group in peak power output, meaning they could produce a few more watts, but really it was only a few (<10). However the one study did find taking anti-histamines impaired submaximal exercise capacity and efficiency.
Anti-histamines also blunted the increase in metabolic and antioxidant enzymes typically seen with exercise. What shocked me personally was that they also completely blocked the beneficial effects of exercise on vascular function and insulin-sensitivity, crucial adaptations that improve cardiovascular health and diabetes risk.
Vascular health and insulin sensitivity are two of the most widely regarded benefits you get with exercise, and it doesn’t take training like an athlete to get them. Even walking gets you substantial improvement if you were previously sedentary. The fact that these responses were clearly altered by OTC anti-histamines is wild.
So, Are We Allergic to Exercise?
And What Can You Takeaway From This?
Clearly, the histamine response to exercise is different from an allergic reaction because it is contained within the active skeletal muscle. So no, we aren’t allergic, and histamine seems pretty important to how we respond and adapt to exercise.
Before you give up completely on your anti-histamines, there are some caveats. These studies always had subjects take the drugs 60min before every exercise session. The drugs used reached peak levels in the blood at 1-2 hours, with a half-life of 3 (H2) and 12 hours (H1). They also used untrained people, which may or may not be you.
You can easily look up on the internet how your specific anti-histamine works, how long it takes to reach peak levels in the blood, and what the half-life is. Once you know that, it may be worth timing your sessions to be as far away as possible to when you consume the drug.
Remember, nothing is free in physiology.
Sean Langan has his PhD in exercise physiology. He is interested in how exercise training rewires our biology and harnessing the intersection of human physiology, technology, research, and coaching to improve human performance. Please contact if there are any topics you’d want to see covered next.